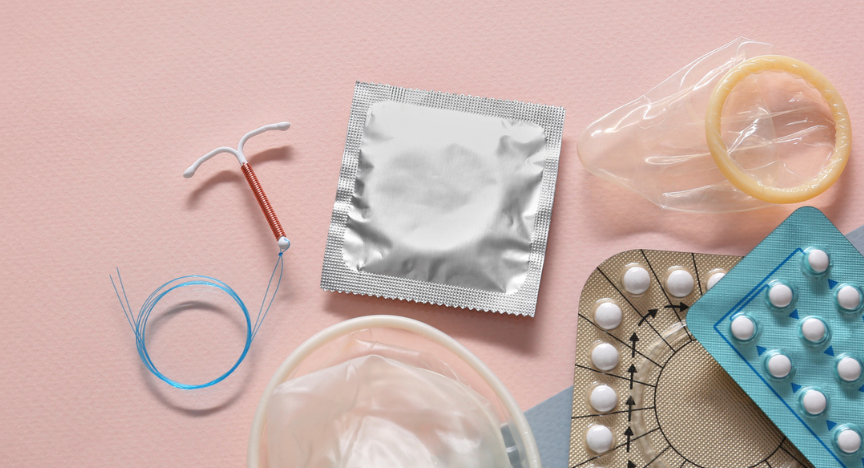
When and how to use emergency
contraception
One of the most prevalent problems we see in therapeutic practice is anxiety
after having sex without protection or when birth control fails. Emergency
contraception (EC) is a dependable and prompt remedy that can substantially
diminish the likelihood of unwanted pregnancy. But it only works if people are
aware of it, use it correctly, and act quickly.
What You Need to Know About Emergency Contraception?
Emergency contraception is meant to stop pregnancy after sex has already
happened. It is crucial to make it clear that EC does not end an existing
pregnancy. Its main job is to stop pregnancy before it starts by delaying
ovulation or inhibiting fertilization.
Emergency contraception is a safe and necessary aspect of reproductive health
care especially when primary contraception has failed or not been utilized. When
used correctly and quickly, emergency contraception is a safe, effective, and
important way to stop unwanted pregnancies. The secret is to be alert, have
access, and make decisions quickly.
When should you think about using emergency contraception?
You should think about EC in the following situations:
• Having sex without protection
• The condom broke, leaked, or slipped
• Missed taking oral contraceptive tablets, especially two or more in a row
• Delay in getting injectable birth
control
• Sexual assault
• Getting the fertile window wrong
In all of these cases, timing is very important. The sooner you use EC, the
better it works.
Different kinds of emergency birth control
There are two primary choices, and the choice relies on when the patient is
eligible for treatment and what they want.
1. Emergency Contraceptive Pills (ECPs)
These are easy to find and utilize a lot.
• Pills that contain levonorgestrel:
Should be administered within 72 hours (3 days), however it might still work
for up to 120 hours. Taking them as soon as possible makes them work best.
• Ulipristal acetate pills: They
work for up to five days following sex, although they are most helpful in the
later window (between 72 and 120 hours). It has a stronger effect on postponing
ovulation.
2. Copper Intrauterine Device (Cu-IUD)
This is the best way to do it, with a success rate of over 99% if you put it in
within five days of having unprotected sex. We typically suggest this to women
who need both short-term and long-term birth control. It keeps you safe for up
to ten years.
How to Properly Use Emergency Contraception?
From a medical point of view, the key is to
use it correctly:
• Take the emergency pill as soon as you
can after having sex
• You can take it at any moment during
your period.
• You don't need to have any tests done before using ECPs.
• If you throw up within two hours, you
should take the dose again.
• Don't start hormonal birth control right
after taking ulipristal; wait at least 5 days.
A visit to the doctor is needed to insert a
Cu-IUD. Before placement, a quick check is done to make sure there are no
contraindications.
Expectations and Effectiveness
• Levonorgestrel pills work up to 85% of
the time if used early
• Ulipristal works better in the 3–5 day
range
• Copper IUD: works more than 99% of the time
Patients should know that EC lowers the risk but does not guarantee that it
will work. It is best to take a pregnancy test if your next period is more than
7 days late.
Side Effects and Safety Profile
Most women, even teens, can safely use emergency contraception. Some common
side effects are:
• Feeling sick or throwing up lightly
• Spotting that isn't regular
• Changes in your period that only last for a short time
• Pain or weariness in the breasts
Most of the time, these symptoms go away on their own and don't need any help.
Things that people worry about a lot
1. Will it have an effect on fertility in the future?
No, there is no proof that emergency contraception affects fertility in the
long run.
2. Is it possible to utilize it more than once?
It is medically safe, but it is not a good idea to use it often because it is
less effective than traditional birth control methods and can mess up your
cycle.
3. Does it keep you from becoming sick?
No, EC does not protect against sexually transmitted infections (STIs). Barrier
protection, like condoms, is still very important.
As a gynecologist, we want to stress that emergency contraception should only
be used as a last resort. Patients who need emergency contraception (EC) more
than once should be told about reliable, long-term birth control methods such
oral pills, intrauterine devices, or implants.
It's also crucial to make sure that patients feel safe asking for help at the
right moment. Delays happen a lot when people are unsure or don't have the
right knowledge which can make things less successful. We not only treat but
also educate ensuring that patients are empowered to make educated reproductive
decisions with confidence and clarity.